This controversial former death row doctor built an empire from treating Georgia inmates
The lives of doctors often revolve around their patients. On a brisk week in early December 2014, Carlo Musso was no exception.
On Tuesday that week, he headed south on Interstate 75 beyond the edges of Atlanta’s sprawl. Not far past where the city fades to country, he pulled off the highway and drove toward the Georgia Diagnostic and Classification State Prison in Jackson.
There, beyond the razor wire and sentry towers, a single patient awaited him. Robert Wayne Holsey, a 49-year-old inmate, had just a few hours left to live.
Nineteen years earlier, Holsey had killed a sheriff’s deputy after a robbery at a convenience store outside Milledgeville. Now, Holsey’s long fight for a reprieve was nearly over. Georgia law required a doctor to oversee his execution. That doctor would be Musso.
What followed that evening resembled a routine medical procedure. A nurse checked Holsey’s veins and set a line. As a lethal dose of pentobarbital was pumped into Holsey’s body, Musso monitored the man’s heartbeat on the electrocardiogram.
Three final words—I love you—floated from Holsey’s mouth toward his sister.
Then, his eyes closed. He drew one last breath. At 10:51 p.m., Musso declared Holsey dead, filled out the death certificate, and headed back toward Atlanta.
Two days later, Musso sat inside a metro Atlanta law firm, where he faced questions about the death of another man. In 2010, Michael Dooling Jr., a 42-year-old painter, had been booked in the Henry County Jail for a probation violation.
Dooling was a smoker who had survived a heart attack and stroke. But the jail had a constitutional responsibility to provide medical treatment to him, as American jails do to all inmates. Jail records show that, not long after he was booked, Dooling informed a physician’s assistant that his doctor had recently told him he needed a pacemaker. But a month into his incarceration, Dooling suffered a heart attack and died. His parents sued the sheriff’s office, as well as CorrectHealth, the private company that treated Henry County inmates. The federal lawsuit also named Musso, CorrectHealth’s founder and president. The lawsuit alleged that his company had failed to provide Dooling with both life-saving surgery and his full set of medications.
By this time in late 2014, the company Musso had started in 2000 had grown exponentially and was now overseeing care for 15,000 inmates at 40 correctional facilities across four states. Lawsuits like Dooling’s were not unusual.
In fact, since Musso became a jail doctor, he and the companies he’d created for each jail had been sued collectively at least 90 times. But in all those lawsuits, CorrectHealth had never lost in court. And they wouldn’t lose this one. (A judge would ultimately dismiss the suit, ruling that Dooling’s parents didn’t show enough evidence that their son’s constitutional rights were violated.)
Musso’s embrace of aggressive strategies to repel lawsuits, along with a broader set of political and personal tactics, have allowed him to engineer an improbable reinvention from an ordinary hospital physician into one of the South’s most influential and controversial doctors. A yearlong Telegraph investigation into CorrectHealth offers a rare view into how Musso built a medical empire that stretches from the Appalachian foothills to the streets of Savannah to the shores of the Gulf of Mexico.
What started as a simple curiosity would lead to the business opportunity of a lifetime. As health care costs soar nationwide, county sheriffs have sought relief from a service they must provide but has nonetheless choked their budgets. Musso was one of the first doctors in Georgia not just to recognize the dysfunction of a system that neither worked for sheriffs nor their patients but also to offer an answer to a fundamental problem that vexed county sheriffs: How do we provide high-quality care on the lowest possible budget?
At the age of 40, Musso traded in the stability and safety of a hospital career to care for patients few others wanted to treat. His second act would enrich Musso — his companies secured over $360 million dollars worth of government contracts since 2000 — and offer a textbook example of how to accrue influence through political lobbying, philanthropic donations, and old-fashioned personal networking. He leveraged jail contacts — and those aforementioned strategies — to expand his suite of services beyond jails to supervising executions and, now, operating a lucrative assisted-living center for former inmates. But Musso’s steady rise would quickly turn the doctor into a lightning rod for controversy. His work would not just exploit a system of lax oversight but also spark a moral and ethical debate over America’s apathy toward an obscure but inalienable right protected by the U.S. Constitution. But the criticisms Musso faced, like the lawsuits and emergencies, were also a part of doing business.
“I know that in our scope we can’t fix every patient’s problem in the time we have, but we can make a positive difference,” wrote Musso, who responded to a partial list of The Telegraph’s questions but declined multiple requests to be interviewed. “That’s what my colleagues and I wake up every day to do.”
An unfunded mandate
When Stanley Tuggle became Clayton County’s sheriff in 1996, he recognized the need for inmate health care but struggled with the burden of what is, in effect, an unfunded mandate. He tried out a private correctional health care provider but grew dissatisfied that its subcontracted general practitioners lacked deep knowledge of his jail’s inner workings. One day in the late 1990s, checking in on a sick inmate at Clayton General Hospital, Tuggle bumped into Musso, a young emergency room physician who lived in Jonesboro. Many of his ER patients — including people who have experienced homelessness, or used drugs — Tuggle also saw in his jail. When Tuggle brought up his health care provider problems, Musso expressed interest in jail medicine. “I told him he was nuts,” Tuggle says. “Why get into medical care in a corrections setting when you’re working in a hospital?” Musso had never before practiced medicine behind bars but understood the importance of correctional medicine: As a boy, he’d watched his father, a doctor, treat inmates. So, when Musso persisted, Tuggle suggested he submit a bid.
After losing the first bid, Musso tailored his proposal to one of Tuggle’s priorities, Tuggle recalls. “I wanted good health care service, but I wanted it within my facility,” Tuggle says. “He built his health care services around the idea of doing everything in-house.” In October 2000 — four months after forming Georgia Correctional Health, LLC — Musso became Clayton’s jail medical provider. Initially, Musso did a little bit of everything: hiring staff, establishing treatment protocols, purchasing medical equipment, and ordering prescription drugs. He also treated inmates, who typically face high rates of chronic diseases like hypertension, asthma, diabetes, and addiction. Though the average jail inmate is locked up for just 25 days, offering a brief window for medical intervention, Musso felt he could “make a tremendous impact on people and on public health,” he told the New England Journal of Medicine in 2006. “I loved it.”
When Clayton built a bigger jail, Tuggle says, Musso helped map out a new infirmary that would bring more medical services such as dental and mental health care in-house. Musso even found a way to move dialysis services to the jail, eliminating the need for deputies to transport patients out of the facility three times each week. Soon, Musso used his Clayton jail experience as inspiration for pitching other counties on his company’s services. His sales proposals would tout his expertise at “cutting costs all while improving the quality and efficiency of health care delivery” inside jails.
Tuggle, for his part, appreciated Musso’s work enough to refer GCH to other sheriffs such as Jeff Wigington of Rockdale County. By 2002, Musso had secured contracts with three more jails—including Wigington’s. Musso had almost entirely moved away from hospital work, focusing on sheriffs, whose support he needed to keep growing his young company. “Anytime I needed him,” said Neal Walden, sheriff of White County, one of Musso’s first clients. “His number was on speed dial.”
Lethal injections
In 2003, Musso received a phone call from a state Department of Corrections official who he has not named publicly. Would Musso oversee Georgia’s lethal injections? the official asked. Musso was uncertain. As a doctor, Musso had been taught to do “no harm” to patients and, as he explains in the 2017 documentary The Sandman, he saw executions as arbitrary, expensive, and unnecessary. But Musso was also curious and asked to visit death row to witness an execution.
The experience left him “incredibly sad,” he told the New England Journal of Medicine. He recalled feeling powerless to comfort the condemned man. Later, Musso read the position of the American Medical Association, which stated a physician “should not be a participant in a legally authorized execution.” But to do nothing, Musso ultimately reasoned, was like abandoning a terminally ill patient.
“When we have a patient who can no longer survive his illness, we as physicians must ensure he has comfort,” Musso told the New England Journal of Medicine. “[A death-penalty] patient is no different from a patient dying of cancer—except his cancer is a court order.” Having a death-row doctor, he felt, would ensure that someone like Robert Wayne Holsey received what Musso called a “painless” death instead of a tortured one, as had occurred in other states, where botched lethal injections had caused inmates to experience convulsions, spasms, and gasp for air.
Musso’s involvement was perfectly legal, though it should have remained secret under state law. But because activists had outed past death-row doctors, Musso was upfront about his role: a job that paid $18,000 per execution to a team of providers that operated under Rainbow Medical Associates, another one of his companies. (Musso donated his portion to a children’s shelter.) Protesters gathered outside his house, challenged his medical license, and asked the AMA to revoke his membership. At times, he conceded in interviews, his role went against his basic reflexes as an emergency physician to prolong life. But he made no apologies.

A ‘dual loyalty’
Any backlash over Musso’s death penalty work did not impede GCH’s growth. Medical ethicist Dominic Sisti says that Musso’s participation showed a “dual loyalty”—a willingness to serve the needs of inmates and their jailer. Between 2002 and 2006, Musso grew the company’s portfolio from four jail contracts to more than 20—including seven in metro Atlanta’s 29-county region—as well as several state prisons. Following Hurricane Katrina, Musso became the medical provider at Jefferson Parish Correctional Center, a large jail south of New Orleans. The out-of-state expansion effectively triggered a companywide restructuring that positioned it for more clients and more growth. He hired in-house lawyers in part to shield the company from legal risk and trained his staff on ways to avoid litigation, according to company records. Musso also folded GCH under CorrectHealth Companies—an umbrella organization that included individual companies for every detention facility, a tactic used to distribute risk. As he shifted away from personally treating patients, Musso spent more of his time tracking inmate medical problems, managing off-site treatment costs, and finding new clients.
Between 2006 and 2016, CorrectHealth doubled its number of jail contracts, overseeing medical care in more than 40 facilities, becoming the largest private correctional medical provider in Georgia and Louisiana while breaking into new markets in Kentucky and Tennessee. By then, the correctional medicine sector had become a $12 billion industry. National companies swallowed regional competitors, morphing into publicly-traded firms like Corizon and Wellpath, which now each oversee hundreds of jails. As more counties outsourced jail medical services—most of Georgia’s 159 counties now rely on for-profit companies—Musso extended a personal touch to his customers. When sheriffs had concerns, Musso answered directly. When they participated in charity golf outings, his company would buy a foursome. Impressed by Musso’s salesmanship, former DeKalb County Sheriff Thomas Brown compared the entrepreneur to the “Col. Sanders” of jail medicine when interviewed by the Atlanta Journal-Constitution in 2011.
Since 2006, Musso gave over $470,000 to political causes through contributions from his corporations as well as he and his wife, Teresa. And he’s not only donated to politicians, but hired them. He’s employed Georgia state Sen. Senator Lester Jackson, a Savannah Democrat, as his dental director. And he’s contracted with Ron Stephens, a Republican state representative, to provide pharmacy services. Between 2012 and 2019, Musso, personally and through his company, has donated more than $27,000 to individual Georgia sheriffs that are his clients.
CorrectHealth contributed at least $250,000 to the Georgia Sheriffs’ Association. (Musso says his sponsorship money went to the Georgia Sheriffs’ Youth Homes, which provide shelter for abused and neglected children.) A 2015 GSA annual report features a photo of two sheriffs handing Musso an award for his “continued generosity of giving.” One of those sheriffs was Donnie Craig, who two years later hired CorrectHealth to treat inmates at his jail in Pickens County. The annual contract is worth over $250,000. Craig said he gave the award as part of his role as then-president of GSYH.
“There’s never been any personal relationship with Dr. Musso and my sheriff’s office,” Craig told The Telegraph. “My relationship is strictly professional.”
Some sheriffs, over time, became CorrectHealth evangelists. Last year, Floyd County Sheriff Tim Burkhalter spoke glowingly of CorrectHealth to a Muscogee County committee tasked with finding a new jail medical provider. The committee ultimately cited positive recommendations in picking CorrectHealth. “I thought it [w]as terrific to see the majority of clients given by CorrectHealth were long-term clients and existing clients,” the committee noted in its report. It didn’t, however, mention that Burkhalter had previously received $3,000 in campaign contributions from CorrectHealth. Burkhalter told the Telegraph that the committee didn’t ask him about the contributions. Last summer, officials in Columbus, Georgia, approved a five-year, $3.4 million contract.
“Over the years [CorrectHealth] did in fact contribute to both my campaign, and many other charitable events, employee benefits and also was instantly responsive when we had any issues with their services,” Burkhalter told the Telegraph. “...I have no qualms about it.”

A new chapter
Sometime around 2016, Musso phased out of his role supervising lethal injections. Leaving behind lethal injections allowed Musso to focus on a new chapter of his medical empire: CorrectLife, a subsidiary of CorrectHealth Companies, builds and operates assisted living facilities designed to serve former prisoners as they age. The first of these is the Bostick Nursing Center, a 280-bed facility in Milledgeville. Musso has said he intends to open additional locations in other states, including one currently in the works in Missouri.
CorrectLife was borne out of Musso’s experience with elderly patients. Even though Georgia’s state prison population is declining, the number of prisoners 60 and older has increased 20 percent since 2011. As those men and women got released, few assisted-living facilities opened their doors, in part because they saw them as a threat. Frail prisoners nearing the end of their sentences often could not be granted early release by the parole board until they had a bed secured. Musso believed that CorrectLife could save taxpayers money while also providing more dignified care to aging prisoners.
For years, Musso had eyed the Bostick Prison, a shuttered 700-bed state prison, as the site of his first CorrectLife facility. Between 2011 and 2012, state records show, Musso discussed with corrections officials a potential deal: The state would invest $8 million in renovations, and Musso would lease the building for $580,000 per month. The following year, after dropping its renovation plans, state officials placed the 16-acre property on the market. Musso, the lone bidder, purchased it for $50,000—half of its appraised value of $100,000. Musso demolished the prison. In its place, he built a $20 million, 110,000-square-foot facility. At the 2014 groundbreaking, Musso was joined by then-Gov. Nathan Deal and state Sen. Burt Jones, a Republican from Jackson, who each lifted shovels of dirt to mark the occasion. (Deal, through a spokesperson, said that Musso’s contributions to Deal’s campaign of nearly $20,000 did not influence his administration’s decisions. Jones did not respond to the Telegraph’s request for comment.)
“It will save us all money,” Deal said of Musso’s project.
Inmate deaths
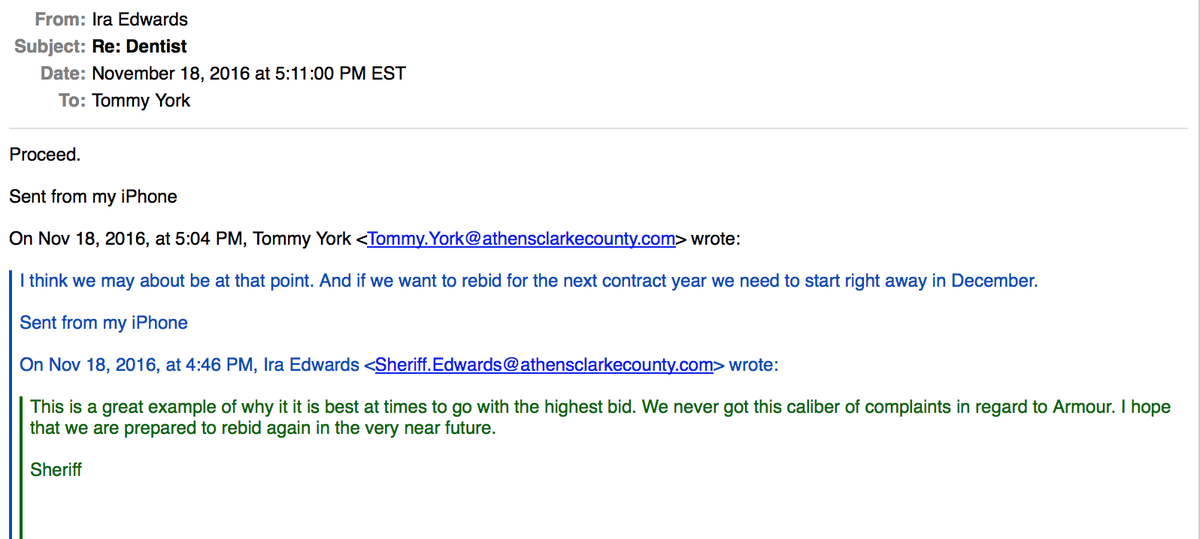
Not all sheriffs have been happy with CorrectHealth’s services. In 2011, DeKalb County fired CorrectHealth, claiming its employees didn’t always show up for work, causing delays to patient care, and asserting that there was too much nursing turnover. In 2015, seven months after Demetrie Jones’s death, Cherokee County bid out its jail medical contract. (The Cherokee County sheriff’s office declined to comment on the cause for the switch.) In 2017, Clarke County rebid its contract after CorrectHealth’s dentist, a subcontractor, failed to come in as scheduled, and Sheriff Ira Edwards wrote in an email that he felt that Musso didn’t adequately address the problem. Edwards ultimately rebid the contract. “This is a great example of why it is best at times to go with the highest bid,” Edwards emailed one of his deputies.
In 2012, a decade into its contract with CorrectHealth and after five years without a single in-custody death, three inmates died at the Rockdale County Jail. One, who had complained of severe abdominal pain, was prescribed a laxative. The inmate, whose name was Albert Wilder, later began vomiting blood and was placed in observation, but he wasn’t given X-rays or any other diagnostic tests. He went into septic shock and died from a perforated ulcer. Wilder’s death was preceded, seven months earlier, by the death of Thomas Colardo. The 66-year-old Conyers resident, who had a platelet disorder that prevented his blood from clotting properly, started bleeding from his nose and rectum. Five days after the bleeding began, a physician ordered a nurse to draw blood, but the procedure didn’t occur for another five hours. Colardo was finally taken to the hospital, where he fell into a coma and died. In a deposition, Sheriff Wigington said that he called Musso after learning of Colardo’s death and told the doctor: “I hope you all are looking into this.”
“[We’re] looking into everything,” Musso replied, according to Wigington’s deposition.
The following year, Wigington lost his re-election bid to current sheriff Eric Levitt, who replaced CorrectHealth. At the time, one of Levitt’s deputies told the county commission that the change was needed because “an ounce of prevention is worth a pound of cure.” Wigington defended CorrectHealth’s performance as the jail’s medical provider. Wigington pointed to another inmate that’s since died under the care of Correct Care Solutions (now part of Wellpath), the company that replaced CorrectHealth. A civil grand jury blamed the man’s death on CorrectHealth’s successor, as well as on the jail staff.
“Every company has issues at some point,” Wigington said. “They changed providers, and they had new deaths.”
Six years after CorrectHealth was replaced, Rockdale is locked in a costly legal battle with Colardo’s attorneys that will likely stretch into 2020. As he closed out one of his most successful years—his companies earned more than $45 million in jail contracts in 2019, and a second CorrectLife facility is in the planning stages—Musso said he wants to look ahead, declining to revisit the circumstances that led to lost contracts or lingering wrongful death lawsuits. “It’s part of being in this business,” Musso wrote, “even when you provide excellent care every day.”
This story is part of a collaboration between The Telegraph and Atlanta magazine. Blau’s series was supported by the Association of Health Care Journalists, the Commonwealth Fund, and the Fund for Investigative Journalism. Margaret Pfohl and Jade Abdul-Malik contributed reporting.
This story was originally published December 13, 2019 at 1:09 PM.