Coliseum’s newest residents get second chance at medical field thanks to Caribbean schools
After Bassem Hanna graduates from medical school this spring, he hopes to give his patients at Coliseum Medical Centers a second chance at life. He knows how valuable second chances can be.
Hanna is not a typical medical school student. He’s one of thousands of aspiring doctors who didn’t quite make the cut to study medicine in the U.S.

Because Hanna didn’t decide to apply to medical school until his junior year of college, he wasn’t as prepared for the application process as his peers who started out on the pre-med track and had already taken all the required courses. Instead of giving up on his dream, Hanna packed his bags and moved to the Caribbean island of Grenada to pursue a medical degree at St. George’s University.
And he’s not alone.
Only 40% of applicants matriculated to U.S. medical schools during the 2017-2018 application cycle, according to the Association of American Medical Colleges. As physician shortages plague communities across the country, international medical schools in the Caribbean hope to help fill the gap.
For decades, Caribbean medical schools have struggled to earn accreditation and esteem in the U.S. Often referred to as second-chance schools, many of these for-profit institutions accept students with lower grades and standardized test scores than their American counterparts.
Though the majority of the more than 60 Caribbean medical schools have yet to match the standards or reputations of their U.S. counterparts, graduation and residency match rates at a select few Caribbean medical schools have increased in recent years. Many of their graduates have gone on to practice medicine at hospitals and clinics here in Middle Georgia.
This summer, a new batch of graduates will start their residencies at Macon hospitals. Hanna is excited to be one of them. He said going to school in the Caribbean gave him the chance to prove he has what it takes to be a doctor.
“It allows you to still pursue your dream of becoming a doctor despite any hardships that you may have faced along the way,” Hanna said. “I just needed that first — that chance to get my foot in the door.”
An alternative option
When international medical schools first emerged in the Caribbean in the 1970s, many medical professionals and academic advisers were wary of the new, for-profit institutions, said Carol Bokros, director of pre-health professional programs at Mercer University. At the time, she said, they catered to students who didn’t meet the academic requirements to gain entry at more prestigious schools in the U.S.
Bokros said many of the Caribbean medical schools lacked resources for students who needed extra academic support, which led to high rates of attrition and low scores on the licensing examinations all students must pass to practice medicine in the U.S.
With time, though, Bokros said, several schools began to improve. Now, the so-called “big four” Caribbean Medical Schools — St. George’s, Ross, Saba University and American University of Caribbean School of Medicine — all boast success rates on par with U.S. programs.
Between 94% and 99% of students at all four schools pass part one the United States Medical Licensing Examination on their first try, their websites report. Their graduates are also more likely to match with U.S. residency programs than in the past, though success rates vary largely between schools.
Last year, 93% of St. George’s graduates were accepted into residencies in the U.S., compared to just 57% of all U.S. citizens who graduated from international medical schools in 2018, according to the National Resident Match Program.
Studies on the success of Caribbean medical schools are mixed. Negative perceptions of such institutions still persist in the medical field, according to a 2018 article in the Canadian Medical Education Journal. Certification rates of students at 12 Caribbean medical schools varied between 28% and 86%, a 2006 study found. Medicare patients treated in U.S. hospitals by graduates of international medical schools had slightly lower mortality rates than patients treated by graduates of U.S. medical institutions, researchers found in 2017.
Bokros sees no reason to dissuade the pre-med students she counsels not to apply to medical schools in the Caribbean, especially if they’ve already faced rejection from U.S. medical schools. The most important thing, she said, is for students to do their research. Bokros suggests prospective students scrutinize schools’ accreditations, costs, curricula, class sizes and success rates to ensure the Caribbean schools they apply to will properly equip them to practice medicine wherever they choose.
“Even though they might not be as competitive to get into, you still have to work really hard. You still have to pass all of these tests and advance,” Bokros said. “It is definitely not an easy way to get into medicine. There is no easy way to get into medicine.”
Graduates join Macon residency programs
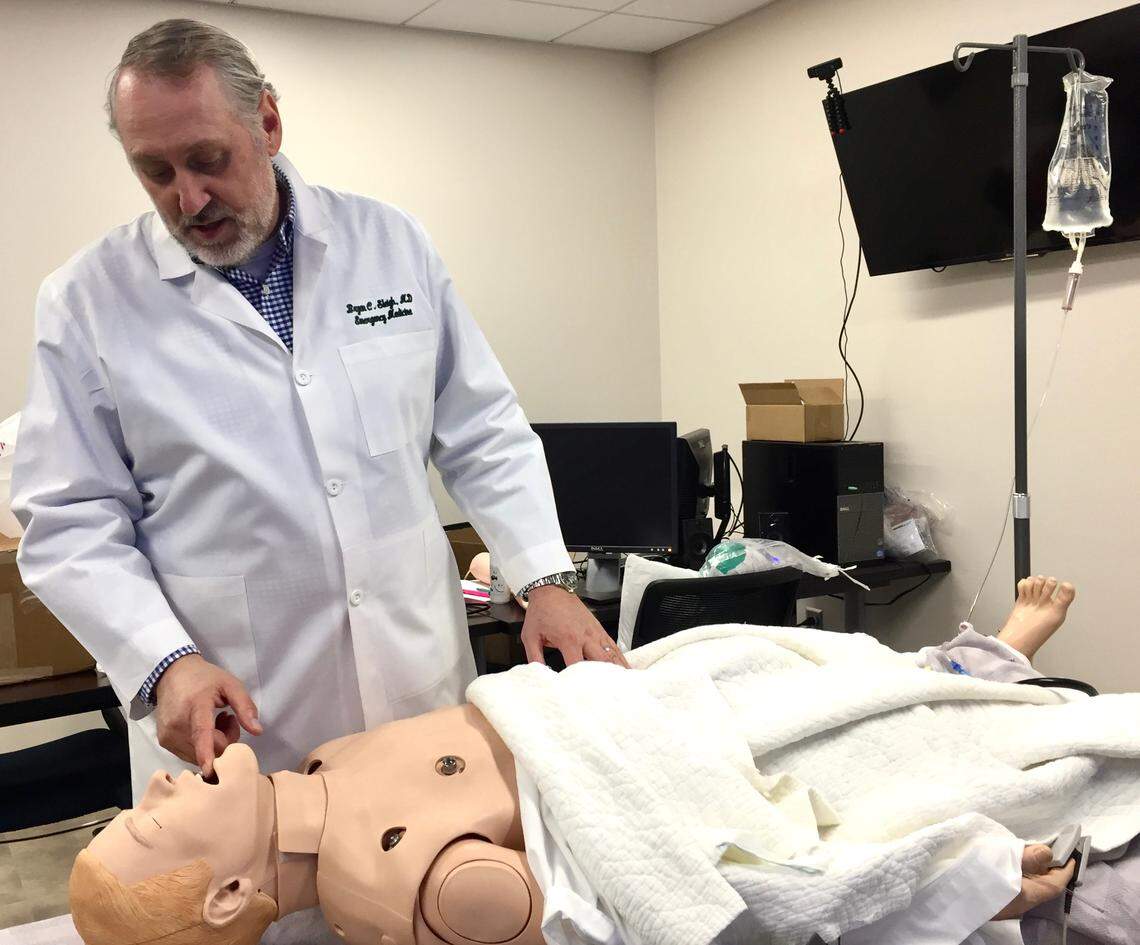
Graduates of Caribbean medical schools play a vital role in Coliseum Medical Centers’ growing residency program, said Dr. Bryan Sleigh, who oversees the hospital’s graduate medical education. Several graduates of Caribbean medical schools, including Trinity School of Medicine and the University of Medicine and Health Sciences, are already residents at Coliseum. Hanna and two other St. George’s graduates will join the ranks this summer.
Residents at Coliseum, which treats patients from underserved and rural areas throughout Georgia, will help to fill the state’s physician shortage, Sleigh said. He hopes his residents will continue to practice in the region, no matter where they studied.
The residency interview process is extensive, Sleigh said.
“If you make it into those programs, that’s kind of a stamp that you’re just as good as everybody else,” he said. “You’re competitive. You’ve been trained well.”
St. George’s President Dr. Richard Olds knows Caribbean medical schools aren’t the right choice for all medical students. If students can get into a U.S. medical school, he said, “Go for it.”
“But there’s a lot of highly qualified medical students that don’t quite make (it) into medical school,” he said.
Olds hopes hospitals and clinics will take a chance on his students and “let them prove to you that they’re great doctors.” The best doctors don’t necessarily score highest on the standardized tests they take when applying to medical school, he said.
“In my over 40 years of being a physician, I’ve never met someone in my life that said the most important quality in my doctor is they got an A+ in organic chemistry,” Olds said.
What patients care about, he said, is that their doctors listen and treat them with care. As a physical medicine and rehabilitation specialist, Hanna hopes to do just that.
When he finishes his residency, Hanna will work with survivors of strokes, spinal cord injuries, traumatic brain injuries and other musculoskeletal disorders, who might have difficulty moving or communicating.
One of Hanna’s patients in medical school could hardly speak after suffering a stroke. He spent nearly an hour with her, helping her act out the answers to his questions so he could make a detailed list of her symptoms and medical history. Hanna said the patient was grateful he took the time to care for her and heed her concerns.
Some doctors save lives, Hanna said. He wants to help patients who suffer from debilitating conditions to live again.
Samantha Max is a Report for America corps member and reports for The Telegraph with support from the News/CoLab at Arizona State University. Follow her on Facebook at https://www.facebook.com/smax1996 and on Twitter @samanthaellimax. You can also join her Facebook group. Learn more about Report for America at www.reportforamerica.org.